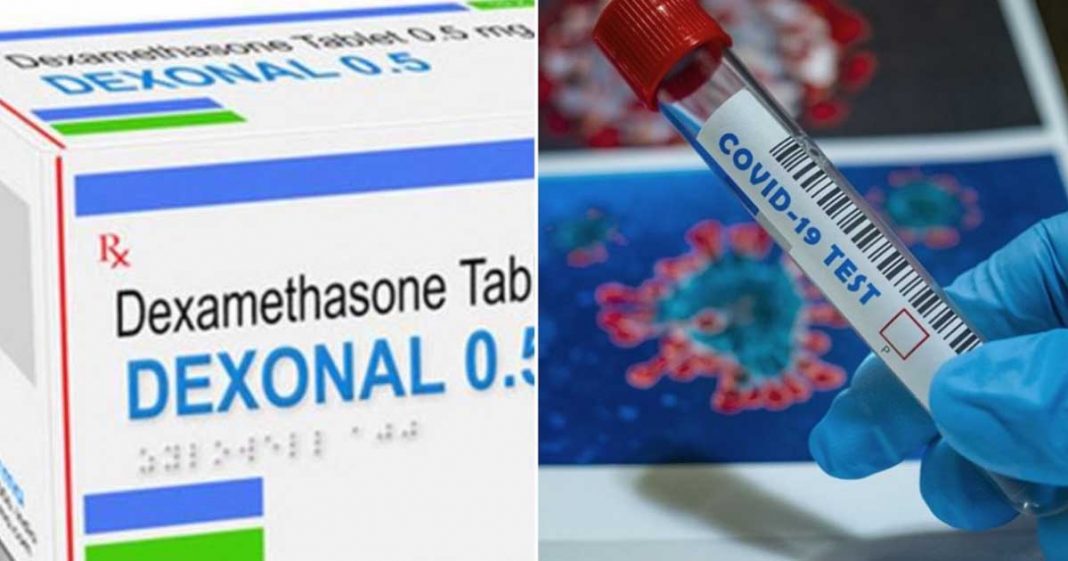
The keenly-awaited full results from a UK trial of the steroid dexamethasone were published Friday, confirming its life-saving benefits for COVID-19 patients on ventilators but suggesting it may cause harm if given too early.
A total of 2,104 hospitalized patients were assigned to receive six milligram daily doses of the medicine for up to 10 days, and 4,321 to receive usual care, with the rate of deaths compared after 28 days.
Dexamethasone used in real life COVID patients
Among patients on ventilators, the rate of death for patients on the drug was 29.3 percent compared to 41.4 percent on those without.
In other words, this group saw a 29 percent reduction in mortality, just under a third.
Read more: Coronavirus Pandemic: This is why prevention is better than Cure
In patients who were given oxygen but through less invasive means, the benefit was smaller — 23.3 percent on dexamethasone died versus 26.2 who were not on it.
However, there was no benefit among the group who weren’t receiving any oxygenation at the time the trial started.
In this cohort, 17.4 percent on the steroid died compared to 14 percent who did not receive it — suggesting the drug increased their mortality risk.
This is because the drug works by suppressing the abnormal immune response that damages the body’s organs, rather than attacking the virus.
In a controlled, open-label trial comparing a range of possible treatments in patients who were hospitalized with Covid-19, patients were randomly assigned to receive oral or intravenous dexamethasone (at a dose of 6 mg once daily) for up to 10 days or to receive usual care alone.
A total of 2104 patients were assigned to receive dexamethasone and 4321 to receive usual care. Overall, 482 patients (22.9%) in the dexamethasone group and 1110 patients (25.7%) in the usual care group died within 28 days after randomization. The proportional and absolute between-group differences in mortality varied considerably according to the level of respiratory support that the patients were receiving at the time of randomization.
Read more: ‘Breakthrough’ steroid treatment for coronavirus praised by WHO
In patients hospitalized with Covid-19, the use of dexamethasone resulted in lower 28-day mortality among those who were receiving either invasive mechanical ventilation or oxygen alone at randomization but not among those receiving no respiratory support.
Dexamethasone ideally should be used sparingly
Speaking in June, leading US scientist Anthony Fauci cautioned that dexamethasone should not be prescribed too soon after a person was infected.
Speaking to AFP in June, leading US scientist Anthony Fauci cautioned that dexamethasone should not be prescribed too soon after a person was infected.https://t.co/Gz42HvoaSU
— The Philippine Star (@PhilippineStar) July 18, 2020
“It had no effect, if not maybe even a suggestion of making things worse early on,” he said.
“This is perfectly compatible with knowing that early on in infection, you need the immune system to suppress the virus.”
The authors of the paper, which appeared in the New England Journal of Medicine, added that getting benefit from the drug “is dependent on a selection of the right dose, at the right time, in the right patient.”
They added that, as far as the COVID-19 illness is concerned, for patients who require oxygen, the abnormal immune response seems more responsible for harm than the replication of the virus in the body.
Read more: Moderna says COVID-19 vaccine in final phase of human trials
But they cautioned that this hypothesis should not be applied to other viral respiratory illnesses, like SARS, MERS and influenza, without further study as they may have different impacts.
Dexamethasone adoption and trial in the UK
Dexamethasone was adopted into UK practice on June 16, the day when the initial results were announced, and is also recommended by the US National Institutes of Health.
#Dexamethasone was adopted into UK practice on June 16, the day when the initial results were announced, and is also recommended by the US National Institutes of Health.https://t.co/laexHL23i5
— Deccan Herald (@DeccanHerald) July 18, 2020
The UK Government-funded trial showed that dexamethasone reduced the risk of death in Covid-19 patients on ventilation by as much as 35% and in patients on oxygen by 20%, reducing the total 28-day mortality rate by 17%. Although the data do identify an improvement in mortality, GlobalData believes that dexamethasone’s place in Covid-19 treatment modalities remains unclear.
Read more: US hoards COVID drug, leaving little for the rest of the world
On its website, the NIH cautions that it isn’t yet known how well dexamethasone might work in combination with the anti-viral drug remdesivir, which has proven beneficial when used alone.
Because they have different mechanisms of action, the combination of these two drugs could be complimentary, with remdesivir slowing damage due to the virus and dexamethasone slowing damage due to a hyper-inflammatory state. This type of scheme is already being considered in trials, specifically with remdesivir and the anti-inflammatory interleukin-6 inhibitor tocilizumab, so the combination of remdesivir and dexamethasone could be attempted.
It adds that patients on the drug should be closely monitored for secondary infections and high blood sugar.
Read more: US gives green light for ‘Remdesivir’ to be used as anti-corona drug
It is also known that use of corticosteroids can also re-activate previous infections that were lying dormant, like the hepatitis B virus or tuberculosis.
AFP with additional input by GVS News Desk