As the government seems to be confident to defeat novel Coronavirus with the help of the citizens’ cooperation, health experts believe that the country may face an acute shortage of ventilators in the coming days.
According to reports, Pakistan does not have enough ventilators due to several reasons. Statistics shared by a health sector expert with The News reflects that public and private sectors of Khyber Pakhtunkhwa (KP) have around 150 ventilators.
Turning 100 ventilators into 400; A thread on the resilience and potential of young creators in Pakistan.
It all started with a story read on 3D printing and how it can contribute to fast tracking the making of life saving equipment amidst an unprecedented global pandemic. pic.twitter.com/hIYRo93aVd
— ZarlashtF NA-251 🪘 (@ZarlashtFaisal) March 27, 2020
In Balochistan, all government hospitals put together have only 49 working ventilators. According to the official record, Punjab’s public sector hospitals have nearly 1,300 ventilators, most of which were procured by the Shahbaz Sharif government in 2016-2018 when it had launched a project for the revamping of tehsil and district hospitals.
National Disaster Management Authority (NDMA) Chairman Lt Gen Muhammad Afzal told the media on Tuesday that he meant to acquire 10,000 additional ventilators over the next few months in order to cope with any health crisis.
Read more: After Saeed Ghani, KP MPA tests positive for Coronavirus
Not only Pakistan, but the entire world is facing a crisis related to medical equipment. In New York, city mayor Bill de Blasio says he needs 15,000. While the vast majority of people who catch the Covid-19 disease experience only mild symptoms, about 6% need hospital care, with older patients at higher risk.
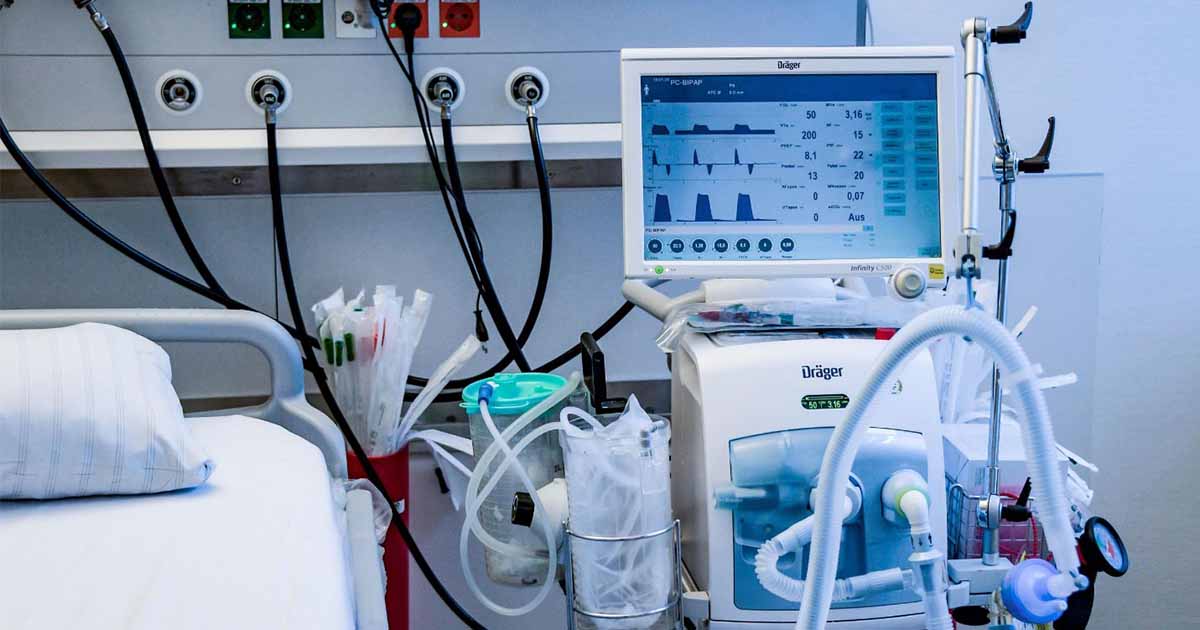
What is a ventilator and how does it work?
A mechanical ventilator is a machine that’s used to support patients with severe respiratory conditions that impact the lungs, including pneumonia.
Before a patient is placed on a ventilator, Day says medical staff – often anaesthetists – will perform a procedure called intubation.
After a patient is sedated and given a muscle relaxant, a tube is placed through the mouth and into the windpipe.
Day says the procedure is routine but, with Covid-19 patients, medical staff need to take extreme precautions to make sure they do not become infected with the virus.
The patient can be sustained for short periods of time using manual forms of ventilation such as using a bag and mask system with oxygen, but usually being attached to a ventilator needs to happen within 30 minutes if critical
“We have people almost in full hazmat suits,” he says.
The breathing tube is then attached to the ventilator and medical staff can adjust the rate that it pushes the air and oxygen into the lungs, and adjust the oxygen mix.
When would a patient go onto a ventilator?
Before deciding to put a patient onto a ventilator, Story says doctors are looking for signs of “respiratory failure”
“The breathing rate will increase, they’ll look distressed, the CO2 in the blood goes up and they can become sedated and confused,” he says.
He says while a normal breathing rate is about 15 breaths a minute, if the rate gets to about 28 times a minute, then this is a signal that ventilation may be needed.
Read more: PM Imran Khan visits Coronavirus quarantine center in Islamabad
Before going on a mechanical ventilator, Prof John Wilson, president-elect of the Royal Australasian College of Physicians and a respiratory physician, says there may be other attempts to increase a patient’s oxygen levels.
These “non-invasive” methods of ventilation can include masks and oxygen tanks.
Story says that with Covid-19, medical staff were looking to avoid non-invasive methods because patients would still cough and splutter, increasing the risk of the virus being transferred to medical staff.
How soon might a patient need a ventilator and for how long?
Ranganathan says once a doctor sees that a patient needs a ventilator, “it is required quickly”.
He says: “The patient can be sustained for short periods of time using manual forms of ventilation such as using a bag and mask system with oxygen, but usually being attached to a ventilator needs to happen within 30 minutes if critical.”
All of that work will be crucial in saving lives if the social distancing measures and community lockdowns don’t stem the flow of patients into critical care
Story says that in severe Covid-19 patients, a life-threatening condition can develop called acute respiratory distress syndrome (Ards) that requires ventilators to deliver smaller volumes of oxygen and air, but at higher rates.
This could mean a patient may need to be on a ventilator “for weeks”.
To avoid complications from the breathing tube going down the throat, Story says a tracheostomy is carried out so the tube can go straight into the windpipe through the neck.
“Patients can be more awake with tracheostomy and the hole just heals itself,” says Story.
“If patients develop Ards they will be in an intensive care unit for weeks and they’ll die without ventilators.”
Why a shortage of ventilators matters, and what’s being done to avoid it.
One of the most obvious ways to avoid a shortage of ventilators, is to reduce the numbers of people catching the disease in the first place. That means following all the health advice, including social distancing and hygiene rules.
In Australia, the Australian Healthcare and Hospitals Association, the Australia and New Zealand Intensive Care Society and the industry minister, Karen Andrews, have all expressed confidence that a shortage can be avoided.
Read more: Funerals in Vienna became online as coronavirus fears ramp up
The Australian government is also investigating whether ventilators used on animals in veterinary clinics could be converted. Sleep apnoea machines and anaesthetic machines are also options.
Story says ventilators used in ambulances could be used as back up.
All of that work will be crucial in saving lives if the social distancing measures and community lockdowns don’t stem the flow of patients into critical care.
Wilson said: “Health care workers responsible for managing severe life-threatening cases like Covid-19 are extremely concerned regarding their ability to use appropriate support for large numbers of patients expected to suffer respiratory failure.
Read more: Coronavirus in Pakistan: Will ignorance & illiteracy let us fight it?
“In essence, this means that many will not be able to be treated with mechanical ventilation and difficult decisions will have to be made by staff, families and patients about the limits of support. There are many ethical dilemmas in this, and none can be easily resolved.”
The Guardian with additional input by GVS News Desk