News Desk |
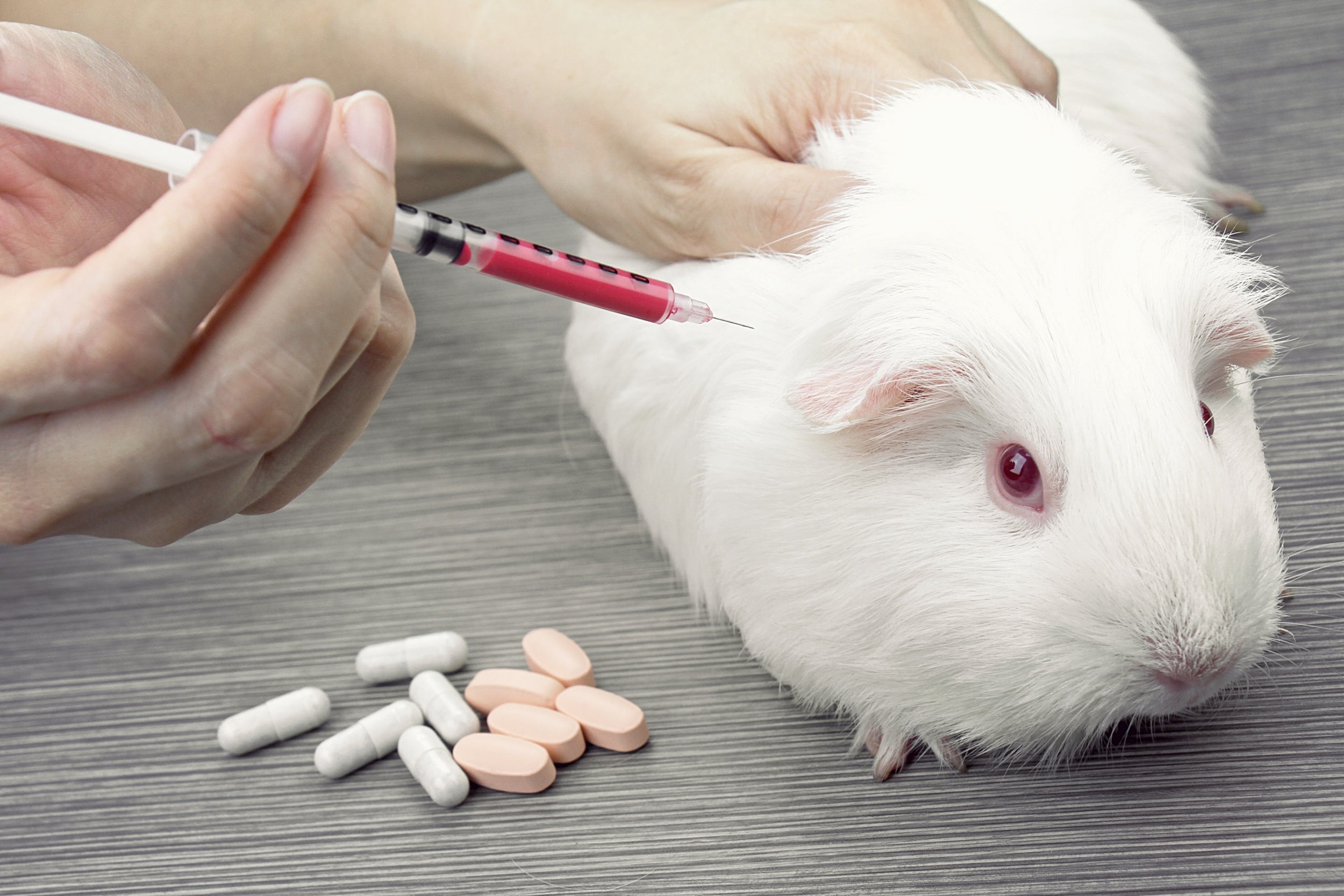
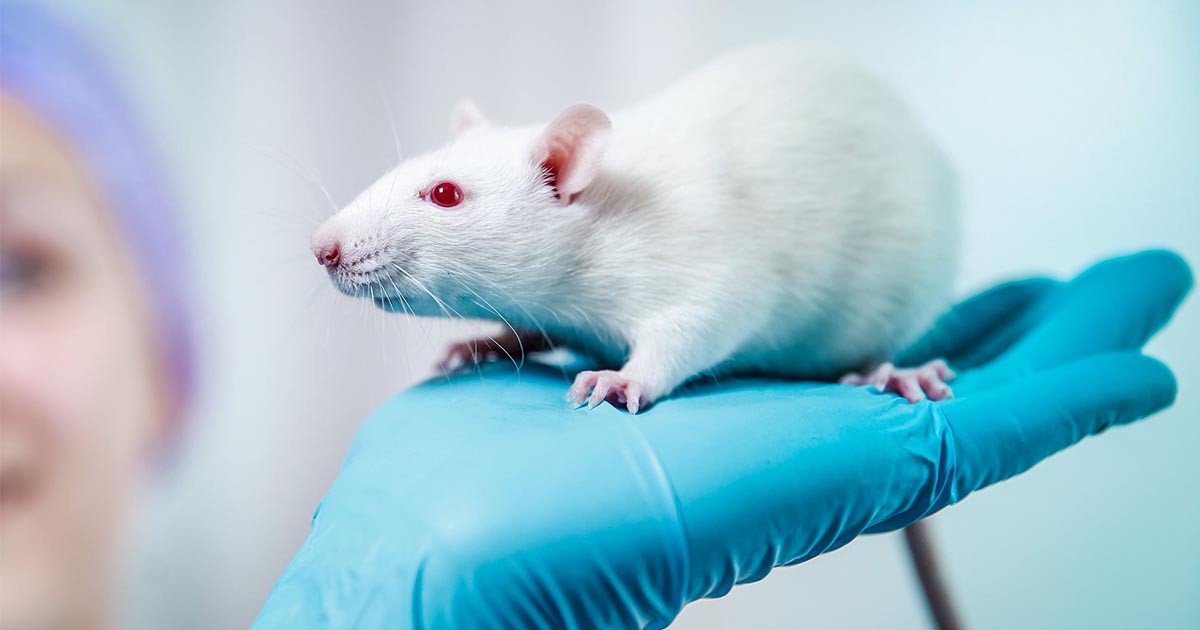
From nutrition to cancer research and studies on metabolism, scientists and journalists alike draw parallels between animals and humans. However, problems can arise when researchers make predictions about human health based on the results of such studies.
Scientists refer to this concept as clinical relevance. Many biomedical grant funding agencies require researchers to justify the use of animal models by predicting how likely the results are to make an impact on human health.

Meanwhile, journalists write catchy news headlines to draw our attention, sometimes failing to critically assess how clinically relevant a study is; or worse, they leave out the fact that scientists performed the work in animals, not humans.
The debate about the clinical relevance of animal models is ongoing, and a Twitter account called @justsayinmice — which encourages social media users to retweet news stories that do not clearly state if results are from an animal model or human volunteers with the caption “IN MICE” — recently fueled it.
Read more: Plastic Kingdom: Fifth largest in the world?
Can we assume that conducting research in animal models will reveal insights about our own health, and who is to blame when a news story includes sweeping statements about clinical relevance?

In this tale of mice and men (in lab coats), we explore how animal studies have contributed to biomedical advances, and why some scientists maintain that animal models harbor no clinical relevance.
Read more: Portuguese artist turns trash into animal sculptures
Animal models date back to ‘2000 BC’
Before we delve into the early days of animal studies, I am going to add in a disclaimer. During my time as a research scientist, before joining Medical News Today, I was involved in several studies that used a large pig model of wound healing.
Although I have made every effort to approach this topic factually, I cannot guarantee that my experiences have not left me without some level of bias.
Read more: Plastic found in deepest ocean’s animals
Through the centuries, animals revealed much of the information we assume as factual today. The key term here is animal model. Maurer and Quimby describe the efforts of several authors to define the “ideal” animal model. “Perhaps the most important single feature of the model is how closely it resembles the original human condition or process,” they explain.

Yet any model will only go so far, they admit: “A model serves as a surrogate and is not necessarily identical to the subject being modeled.”
Read more: Climate change forces Arctic animals to shift feeding habits: study
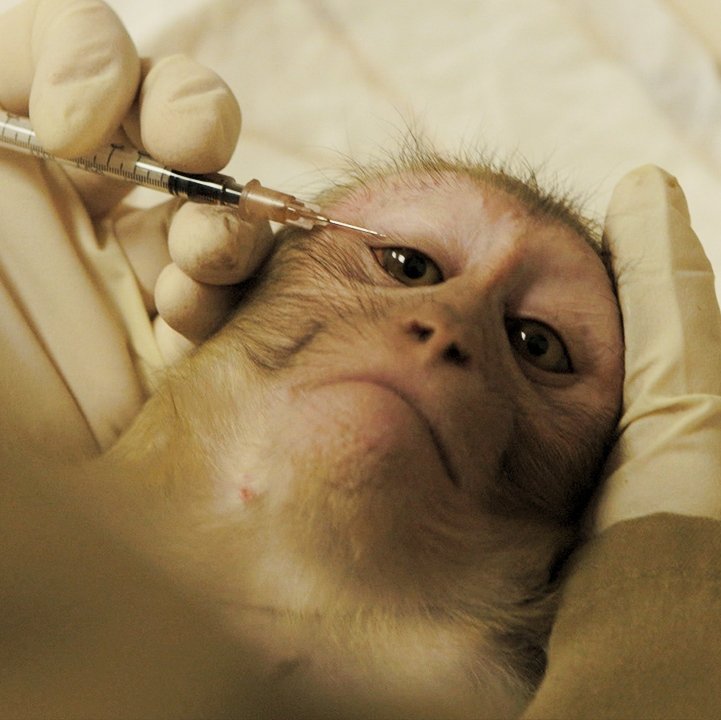
In a 2018 paper in the Journal of Translational Medicine, Pandora Pound, from the Safer Medicines Trust in the United Kingdom, and Merel Ritskes-Hoitinga, from Radboud University Medical Center in Nijmegen, the Netherlands, argue that “preclinical animal models can never be fully valid due to the uncertainties introduced by species differences.”
Their article has a particular focus on the pharmaceutical industry, which has a significant requirement for animal studies at the stage before a drug enters clinical trials. Without such preclinical models, it is not currently possible to test new drugs in humans.